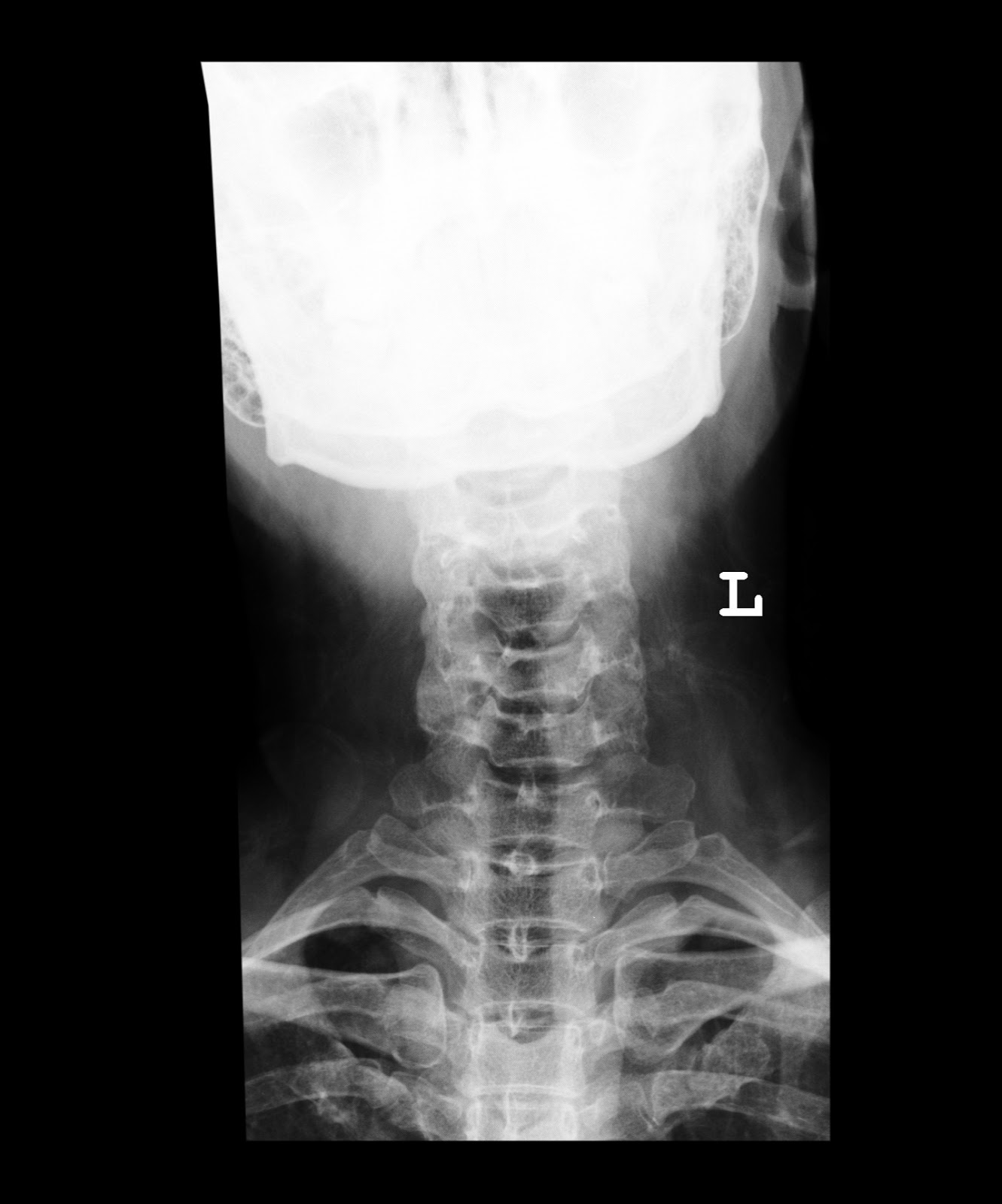
Left paratracheal and aortopulmonary nodes also frequently enlarged, but harder to identify The Scadding criteria have been used, despite limitations, to stage sarcoidosis for decades.Ĭlassic nodal constellation reflects relatively high sensitivity of chest x-ray for adenopathy in these nodal stations The radiograph may appear normal despite the presence of pulmonary granulomas histologically (5-10% of cases). alveolar sarcoidosis) - less commonĬhest x-ray is less sensitive than CT for thoracic manifestations of sarcoidosis. Wide spectrum of pulmonary parenchymal changes:Īirspace opacities/consolidation (e.g. usually without mass effect on adjacent structures (e.g. Isolated anterior/posterior nodal enlargement uncommon - almost always occurs in combination with middle mediastinal and hilar involvement 3Ītypical patterns more common in patients presenting ≥50 years of age 3 Unilateral hilar enlargement without mediastinal involvement rare (1-3%) 3 Hilar nodes almost always involved (isolated middle mediastinal adenopathy rare) Symmetric hilar and mediastinal lymphadenopathy (>75%) 1,3 In addition, it is essential to understand that imaging findings are non-specific or atypical in 25-30% - sarcoidosis is often termed the "great mimicker" 7.Īlthough there is a large spectrum of thoracic imaging findings, the most typical manifestations include: Imaging evaluation can be tricky, as the manifestations are variable and depend on the stage of disease on both x-ray and CT 1-3. The granulomas may resolve spontaneously or progress to fibrosis.īoth chest radiograph and CT are commonly used to evaluate for thoracic sarcoidosis. Microscopically, the granulomas are typically non-caseating and coalescent. Thus, on gross examination, multiple pulmonary granulomas occur in a characteristic lymphatic and perilymphatic distribution. This distribution is one of the most helpful features in recognising sarcoidosis pathologically and is responsible for the high rate of success in diagnosis by bronchial and transbronchial biopsies 10. Sarcoid granulomata mainly occur in a distribution along the lymphatics in the bronchovascular sheath and, to a lesser extent, in the interlobular septa and subpleural lung regions. Obstructive components are usually seen in patients who also smoke, and are primarily attributable to the later 6. Respiratory function tests tend to demonstrate a restrictive pattern with reduced lung volumes and reduced diffusion capacity. Löfgren syndrome is an uncommon but specific acute presentation with a better prognosis. erythema nodosum, lupus pernio, scars, plaques) 3. cough and dyspnoea) or skin changes (e.g. The remainder present with either respiratory symptoms (e.g. Approximately 50% of patients are asymptomatic. Clinical presentationĬlinical presentation is variable. Patients between 20 and 40 years of age are most commonly affected, although lung involvement can be seen at any age 1. There is a slight female predominance, particularly among African-Americans. Pulmonary manifestations are present in ~ 90% of patients.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
